WELCOME
Welcome
Your Optometrist In St. George, Utah
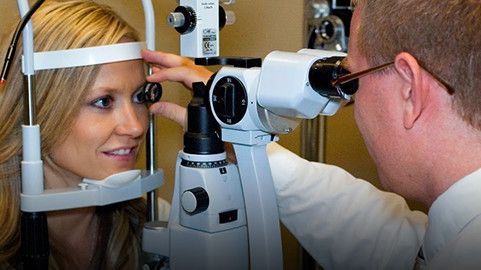
We believe LIFE is all about YOUR vision. When you come see us here at Paradise Canyon Eye Care in St. George, Utah, we’ll sit down with you to discuss your wants, needs and concerns and answer any questions that you might have about eye care. Whether your concern is about glaucoma, cataracts, macular degeneration, diabetic retinopathy, or other eye disease or eye condition or you simply need eye glasses and contact lenses that help you see and feel your best, Dr. Joseph Fife is the eye doctor for you and your family. We’ll create a personalized solution for you and your eyes all while making sure that we remain within your budget. Our team is highly experienced working with both children and adults.
SERVICES
Featured Services
At Paradise Canyon Eye Care, Dr. Joseph Fife and our entire Paradise Canyon Eye Care team are committed to providing advanced vision care for the whole family in a professional and welcoming environment. As a leading optometric practice in St. George, we offer a wide array of primary eye care services to fit you and your family’s needs, including:

Neurolens
The first and only contoured prism lens shown to relieve the painful symptoms of today’s hardworking eyes.
Learn More
Dry Eye
An estimated 40 million people in the U.S. are affected by dry eye.
Learn More

Scleral Lenses
Some types of contact lenses are known as speciality lenses.
Learn More

Advanced Optometric Solutions
As a leading optometric practice in St. George, we offer a wide array of primary eye care services to fit you and your family’s needs, including:
Learn More

Meet Dr. Joseph Fife
Our St. George Eye Doctor
Dr. Fife is founder and CEO of Paradise Canyon Eye Care. Paradise Canyon Eye Care provides personalized, patient-centric eye care service to the southern Utah communities in and around St. George, Utah. Over 6,000 patients hail from 5 US states and 5 countries. Dr. Fife received his Doctor of Optometry degree in 2001 from Southern California College of Optometry and was elected a member of Beta Sigma kappa International Optometric Honor Society for graduating with honors.
Learn More
Meet Our Team
Optical Boutique
Designer Frames






























- Pepperoni
- Sausage
- Cheese
- Mushrooms
- Chicken
- Pepperoni
- Sausage
- Cheese
- Mushrooms
- Chicken










What Our Patients Say
Patient Reviews